ACO utilization & cost evaluation
ACO Insight
Get better answers from your data
Milliman’s ACO Insight reporting interface provides claims data insights to identify opportunities for efficiently managing the cost and quality of care provided to Medicare, Medicaid and commercial ACO populations.
Users can analyze utilization patterns over time and drill into the detail of individual patient cohorts to identify cost savings opportunities. This web-based data visualization tool contains a number of pre-defined data views along with benchmarks, where available. Users can log on to the interface at their convenience and access personalized, comprehensive reports prepared by Milliman.
Interactive dashboards give you full control
ACO Insight allows the user to control the views of data presented using a simple and straightforward set of predefined filters customized for each client population.
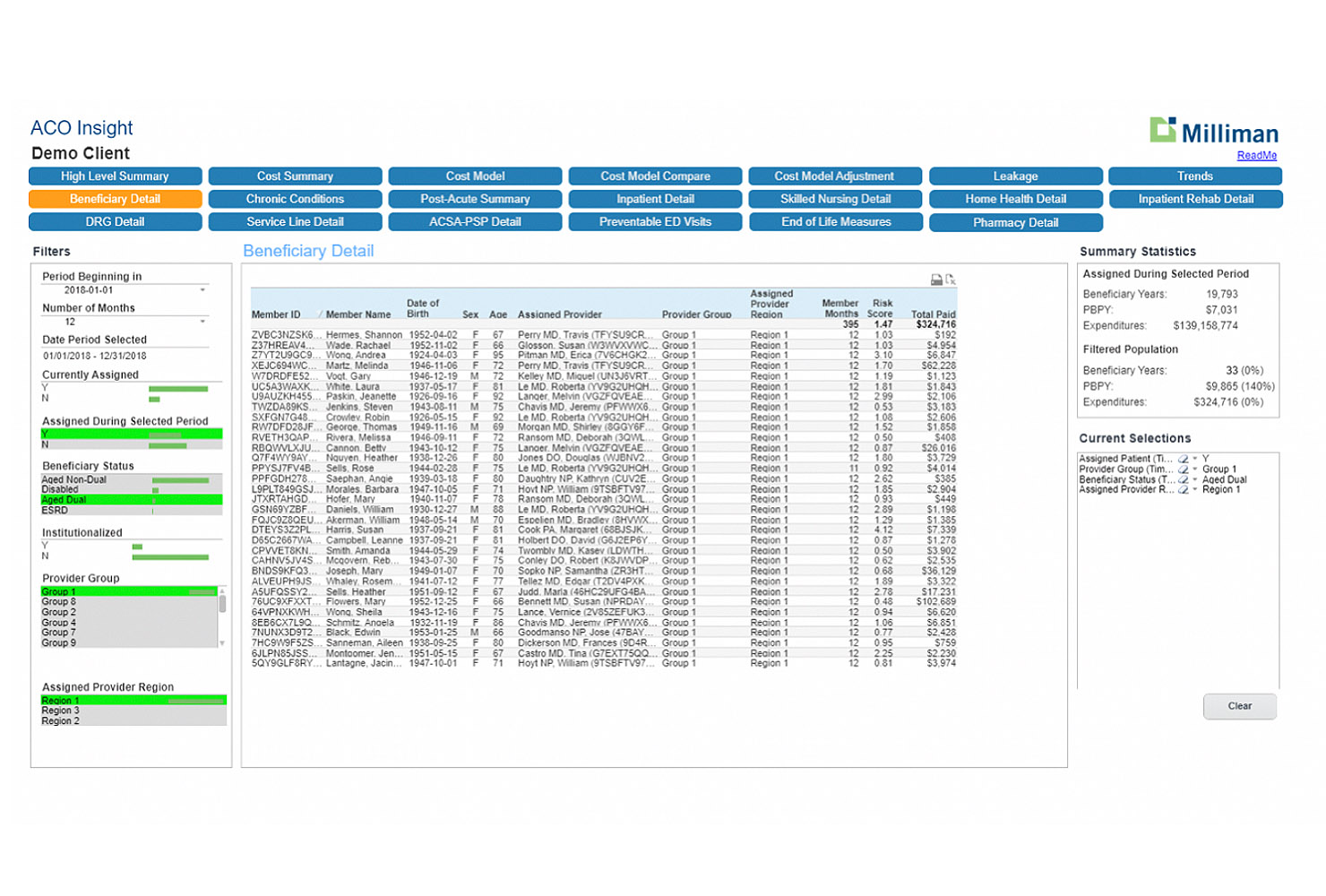
Multiple ways to view your data
ACO Insight provides various reporting views that the user has the ability to control through numerous filters. The user can filter data based on time period, demographic characteristics, provider group or region, or other criteria.
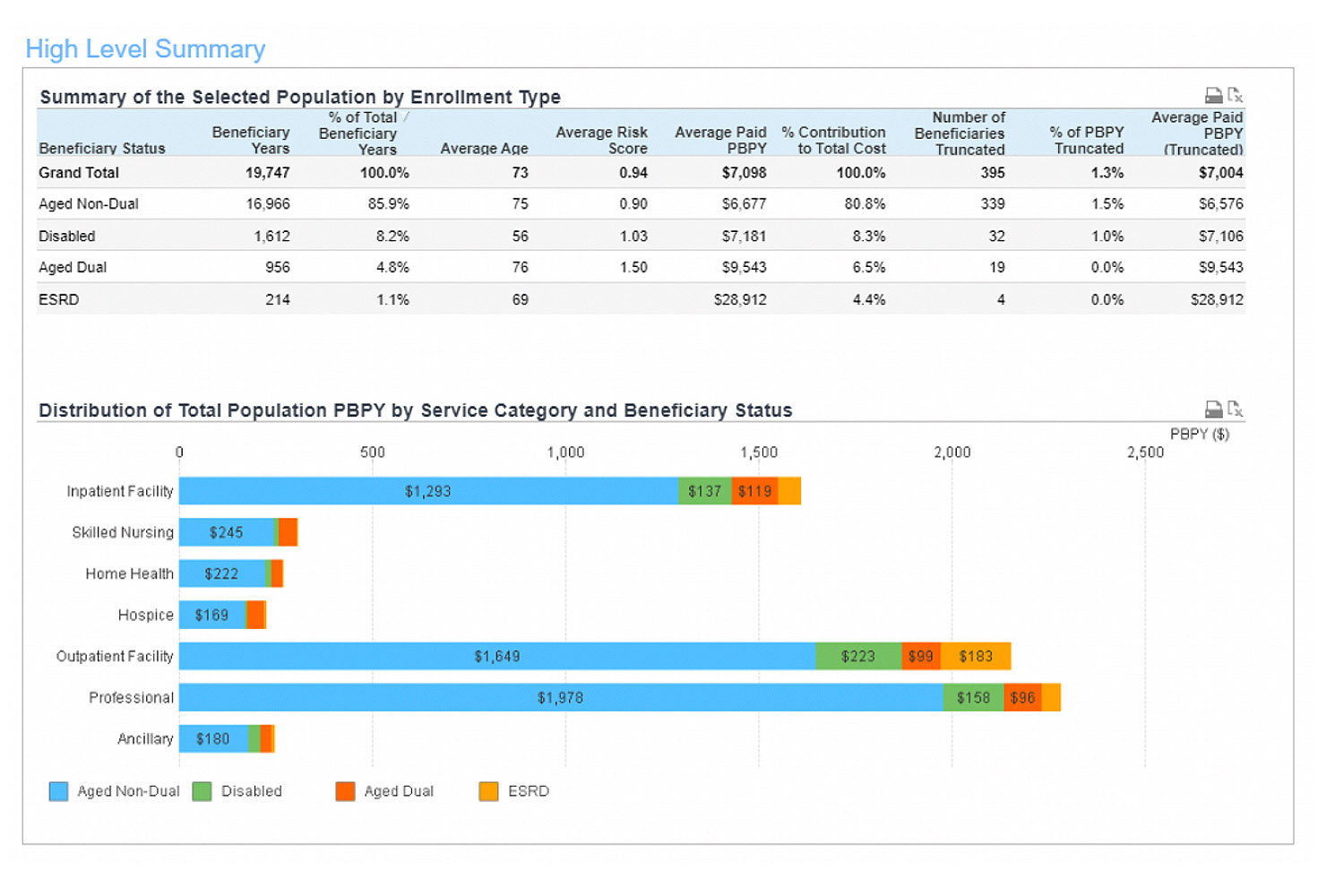
High level summary
The high level summary includes population characteristics such as counts, risk scores, and annual per member/beneficiary costs.
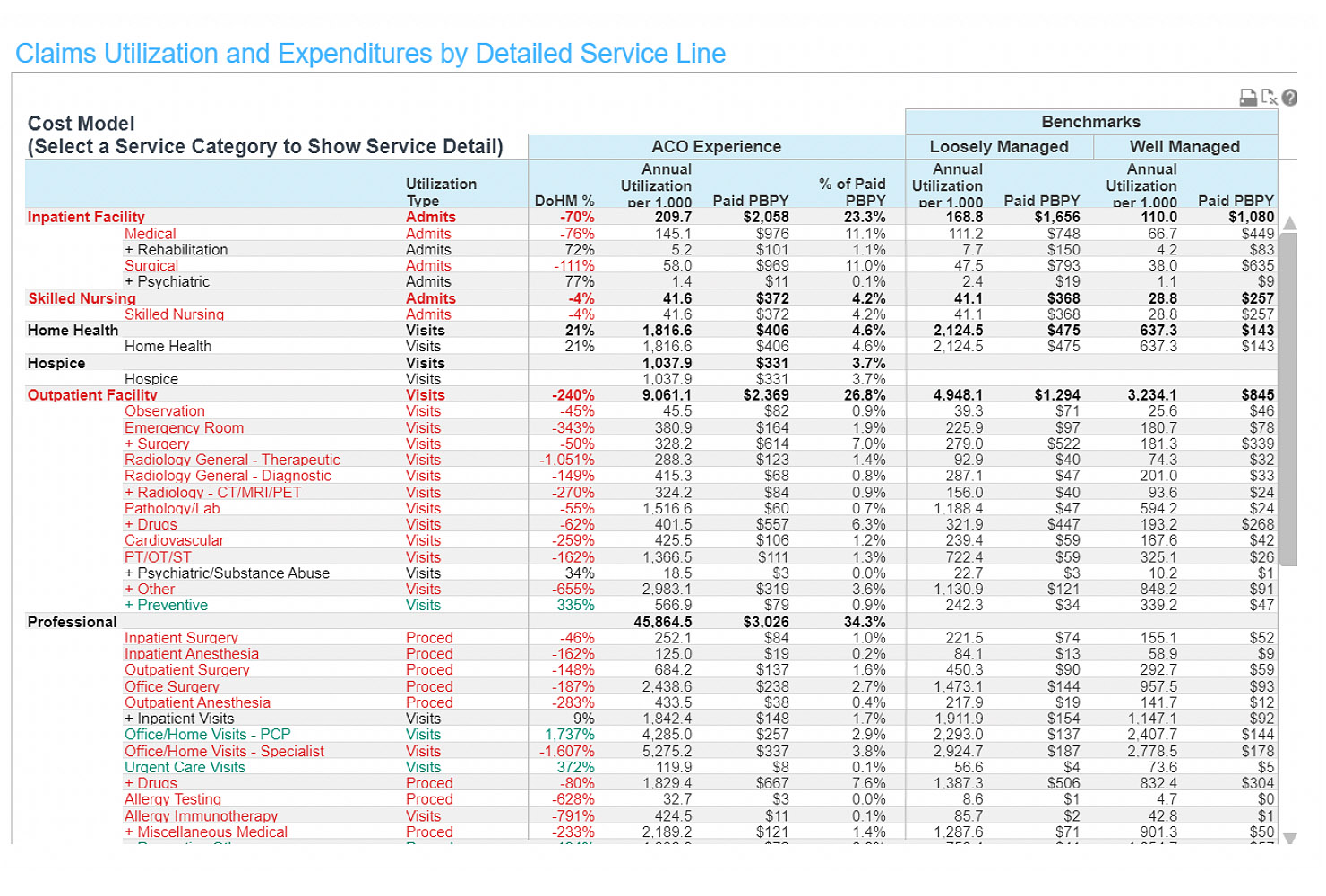
Claims utilization & expenditures
Comparing utilization of a selected service category to benchmarks provides an ACO with the ability to evaluate whether there is a feasible opportunity to reduce utilization for that service. In order to credibly compare ACO performance to benchmarks, the benchmarks are risk- or demo-adjusted at the service category level to reflect the risk/demographic profile of the ACO’s assigned population.
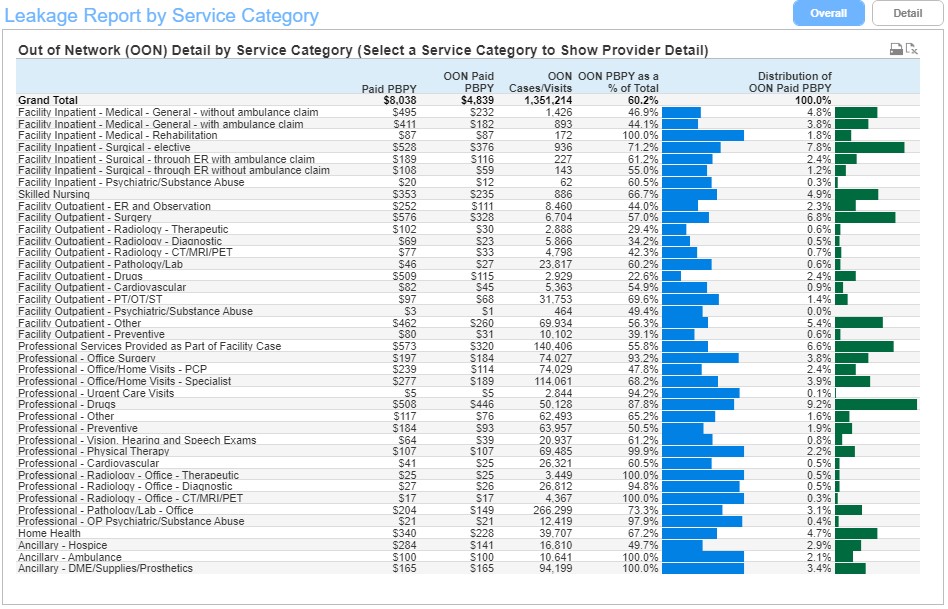
Leakage by Service Category
This report allows users to identify the services with high out-of-network utilization. Users can drill into particular service categories to examine the providers patients are seeing out of the network or ACO.
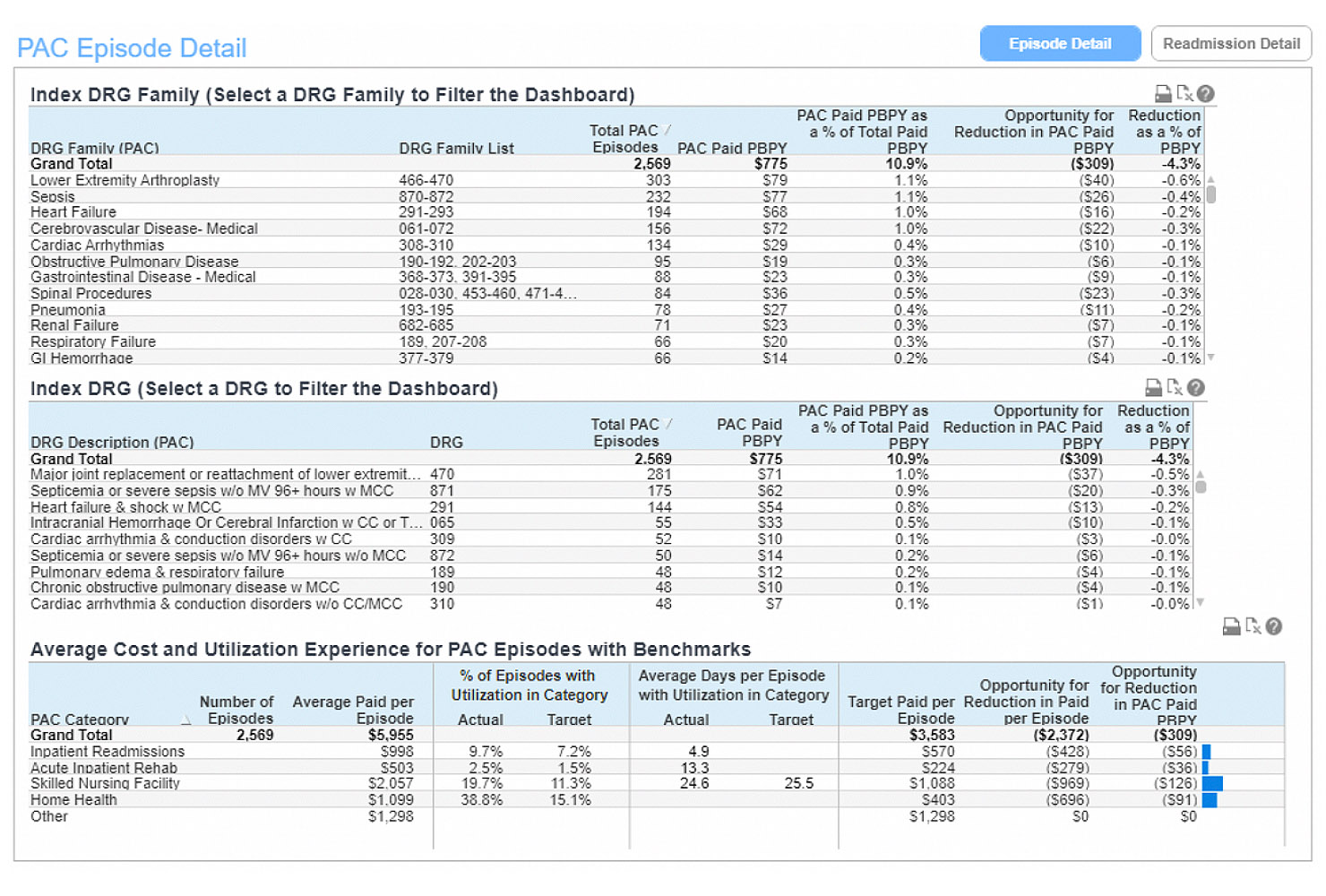
Post-Acute Care (PAC)
These reports provide details on PAC episodes of care, with views that include PAC episode costs by anchor hospitalization DRG, utilization and costs by PAC category (e.g., skilled nursing facility, home health) and comparisons to Milliman-developed PAC benchmarks. Users can drill into PAC categories or episodes by DRG family to better understand not only what is driving costs but also the potential opportunity for savings.
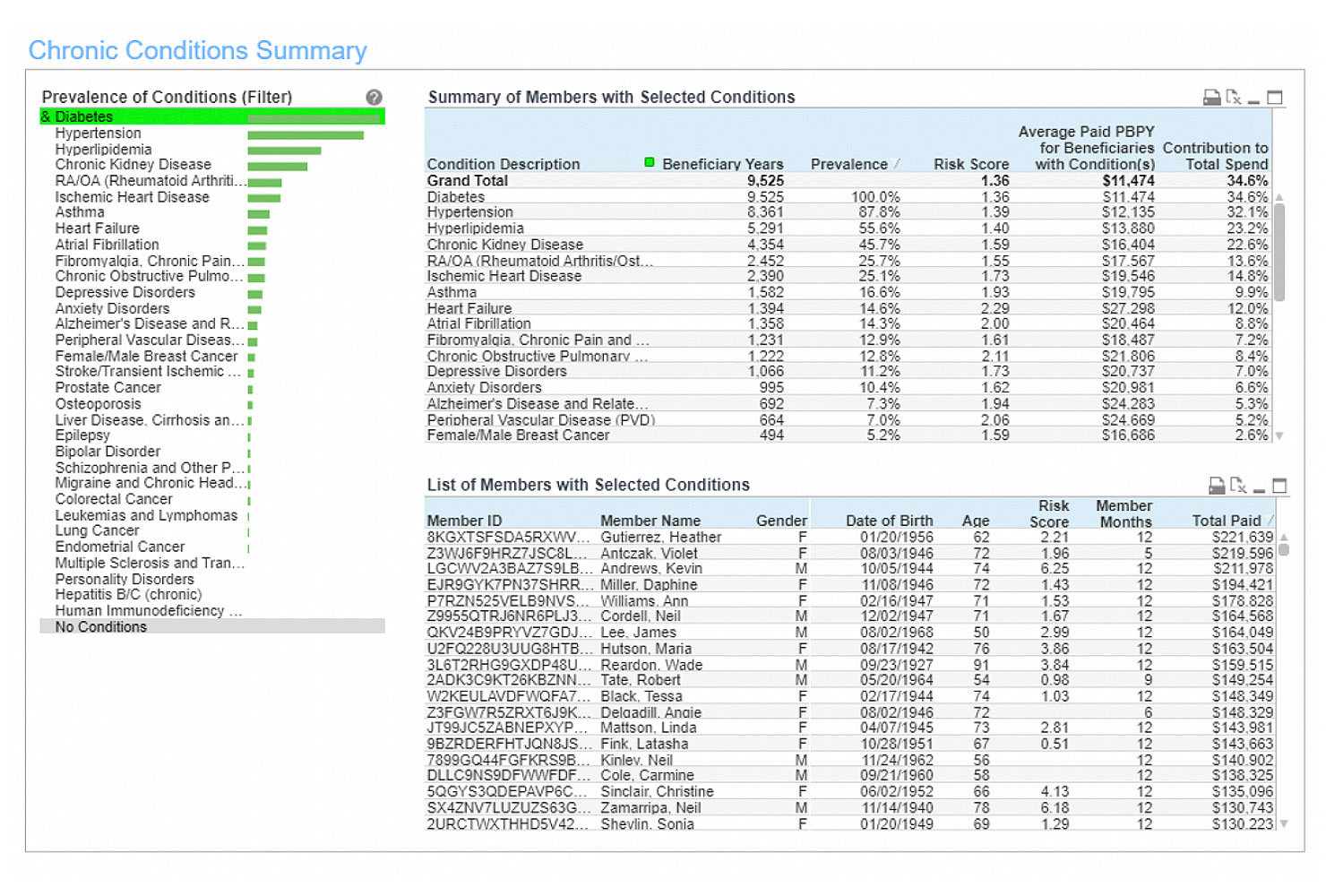
Chronic conditions
Patients are flagged with common chronic conditions or potentially disabling conditions through historical claims-based algorithms based on the CMS Chronic Condition Warehouse (CCW) that look for specific diagnosis codes in the prior 12 months. The reports provide population-based statistics such as prevalence, risk scores and costs for these cohorts as well as individual member detail. Users can view any report within ACO Insight for a particular cohort of patients based on selected chronic condition(s).
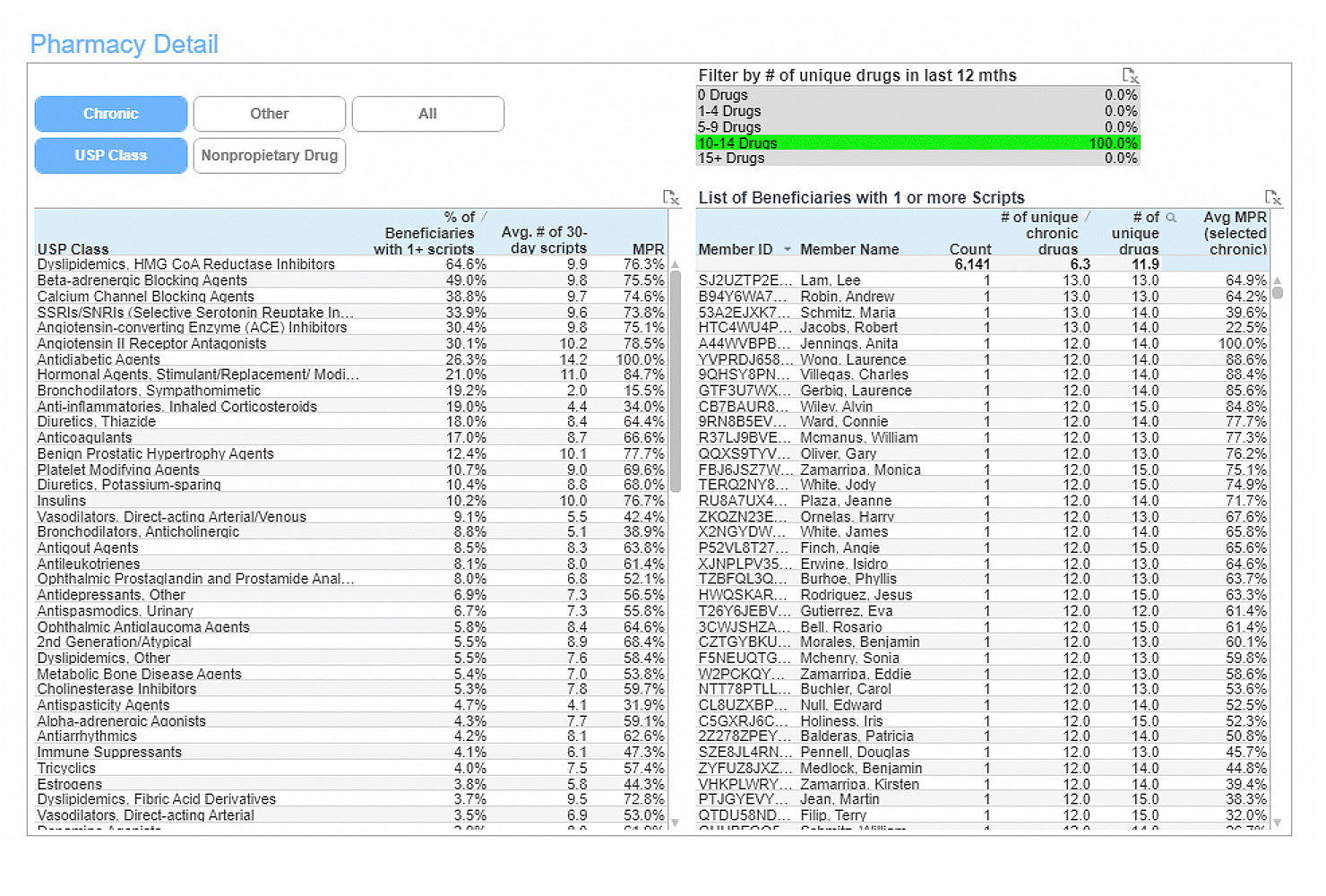
Prescription drugs
The pharmacy dashboard details drug utilization, adherence and cost, if available, for prescription drugs. Drugs are classified as chronic or non-chronic and grouped by drug class or non-proprietary drug name. These pharmacy reports allow users to analyze high drug utilizers as well as utilizers who are less adherent to their drug regimen.
Services related to ACO Insight
Actuarial consulting: healthcare
Get a handle on the complexity of estimating healthcare financial risk with the industry's leading actuarial services firm.
Advanced analytics for accountable care organizations
Answer key business questions with our in-depth understanding of risk-sharing contracts, advanced analytics, and modeling.
Financial projections
We perform financial feasibility projections and can perform ongoing financial projections to assist in financial reporting.
Medicare ACOs
Implement effective alternative payment strategies in collaboration with Medicare, including shared savings arrangements.
Stop loss/reinsurance/capital requirements
Choose stop-loss coverage that meets your needs and budget as risk-sharing payment models proliferate.
Benchmarking
Identify areas of strength and gaps in performance with benchmarking reports that provide actionable advice.
Data analytics support, contract reconciliation/settlements
Our proprietary software, along with consulting services, will help you improve existing processes and create useful new solutions.
Physician incentive models and surplus distribution
We can assist health systems in developing the distribution model and ensuring it is tailored appropriately to the goals of each system.
Operational consulting
Milliman healthcare consultants with in-depth knowledge of Medicare Advantage programs provide services to support Part C and Part D plan sponsors in operating their plans.
Value-based reimbursement strategy
Reduce risk and increase revenue from the patient to the system level, including population health management and financial strategy.
Products related to ACO Insight
MedInsight
Adopt the healthcare industry’s leading platform for data warehousing and healthcare analytics.
ACO Care Management Impact Model
Model, establish, and measure medical management outcomes to achieve performance targets and make sound decisions.
Bundled Payment Reporting Interface
Manage episodes of care under Medicare bundled payment models using the same logic and claims data employed by CMS.
Want to learn more about ACO Insight?
Industry insight
Alternate payment models
Explore all expert thinking from Milliman related to alternate health care payment models